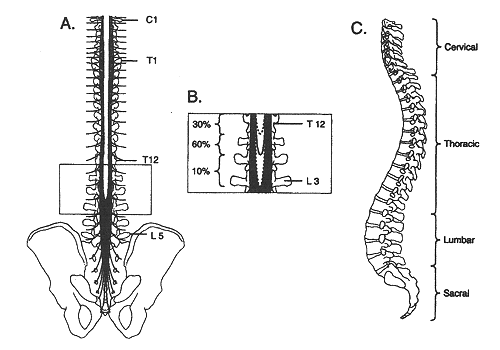
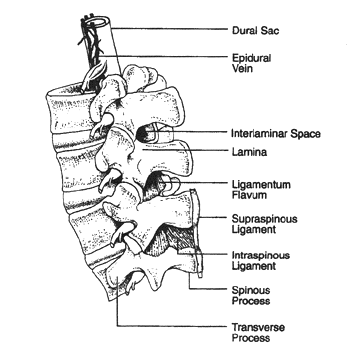
Epidural & Spinal Anesthesia: Understanding the FactsWomen's Health & Education Center's Contribution. We hope that you, the reader, will benefit from this symposium on pain management during labor and delivery, and we trust that it will improve your understanding. Epidural & spinal anesthesia (regional anesthesia) has become more popular recently, because they are well suited to pain management during labor. It offers the most effective form of pain relief and is used by most women in the United States. There are no absolute indications for epidural anesthesia. However, there are clinical situations in which patient preference, patient physiology, or the surgical procedure makes epidural anesthesia the technique of choice. Thus, epidural anesthesia is an indispensable part of modern anesthetic practice, and every anesthesiologist should be adept at performing this procedure. Proficiency in epidural anesthesia requires a thorough understanding of the anatomy of the spine and spinal cord. Epidural anesthesia can be used to extend analgesia into the postoperative period or to provide analgesia to non-surgical patients. Spinal and epidural anesthesia each have advantages and disadvantages that may make one or the other technique better suited to a particular patient or procedure. The purpose of this document is to understand indications, contraindications, techniques and areas of future research in regional anesthesia (epidural and spinal anesthesia). In obstetric patients, regional analgesia refers to a partial to complete loss of pain sensation below the T8 to T10 level. In addition, a varying degree of motor blockade may be present, depending on the agents used. The spine consists of 33 vertebrae (7 cervical, 12 thoracic, 5 lumbar, 5 fused sacral, and 4 fused coccygeal). The vertebral bodies are stabilized by five ligaments that increase in size between the cervical and lumbar vertebrae. In most obstetric patients, the primary indication for epidural analgesia is the patient's desire for pain relief. The American Society of Anesthesiologists (ASA) and the American College of Obstetricians and Gynecologists (ACOG) recommend that third-party payers should not deny reimbursement for regional analgesia and anesthesia because of an absence of other medical indications. The epidural space is the space that lies between the spinal meninges and the sides of the vertebral canal. It is bounded cranially by the foramen magnum, caudally by the sacrococcygeal ligament covering the sacral hiatus, anteriorly by the posterior longitudinal ligament, laterally by the vertebral pedicles, and posteriorly by both the ligamentum flavum and vertebral lamina. The epidural space is not a closed space but communicates with the paravertebral space by way of the intervertebral foramina. The epidural space is shallowest anteriorly where the dura may in some places fuse with the posterior longitudinal ligament. The space is deepest posteriorly, although the depth varies because the space is intermittently obliterated by contact between the dura matter and ligamentum flavum or vertebral lamina. Contact between the dura mater and the pedicles also interrupt the epidural space laterally. Thus, the epidural space is composed of a series of discontinuous compartments that become continuous when the potential space separating the compartments is opened up by injection of air or liquid (1). The spinal meninges consist of three protective membranes (dura mater, arachnoid mater, and pia mater) that are continuous with the cranial meninges. The dura mater is the outermost and thickest meningeal tissue. The inner surface of the dura mater abuts the arachnoid mater. There is potential space between these two membranes called the sub-dural space. Occasionally, drug intended for either the epidural space or the subarachnoid space is injected into the sub-dural space. Sub-dural injection has been estimated to occur in 0.82% to 10% of intended epidural injections. The arachnoid mater is a delicate, avascular membrane composed of overlapping layers of flattened cells with connective tissue fibers running between the cellular layers. The spinal pia mater is adherent to the spinal cord and is composed of a thin layer of connective tissue cells interspersed with collagen. The pia mater also gives rise to the dentate ligaments, which are thin connective tissue bands extending from the side of the spinal cord through the arachnoid mater to the dura mater. These ligaments serve to suspend the spinal cord within the meninges. Identifying individual vertebrae is important for correctly locating the desired interspace for epidural and spinal blockade. The spine of C7 is the first prominent spinous process encountered while running the hand down the back of the neck. The spine of T1 is the most prominent spinous process and immediately follows C7. The 12th thoracic vertebra can be identified by palpating the 12th rib and tracing it back to its attachment to T12. A line drawn between the iliac crests crosses the body of L5 or the L4-5 interspace. Midline insertion of an epidural needle is least likely to result in unintended meningeal puncture. Spinal and epidural anesthesia should be performed only after appropriate monitors are applied and in a setting where equipment for airway management and resuscitation are immediately available. Before positioning the patient, all equipment for spinal block should be ready for use (e.g. local anesthetics mixed and drawn, needles uncapped, prep solution available). Spinal and epidural needles are named for the design of their tips. Epidural needles have a larger diameter than spinal needles to facilitate the injection of fluid or air when using the "loss-of-resistance". A catheter is placed in the epidural space, allowing for continuous epidural infusion of local anesthetic agents or narcotics. The advantage of this method is that medication can be titrated over the course of labor as needed. In addition, epidural catheters placed for labor analgesia can be used for cesarean delivery or postpartum tubal ligation. Modern epidural preparations that combine a low-dose local anesthetic, such as bupivacaine, levobupivacaine, or ropivacaine, with an opioid agonist are preferred because they decrease motor blockade and result in an increased rate of spontaneous vaginal delivery (2). Careful attention to patient positioning is critical to successful spinal puncture. Using the iliac crests as a landmark, the L2-L3, L3-L4 and L4-L5 interspaces are identified and the desired interspace is chosen for needle insertion. Interspaces above L2-L3 are avoided to decrease the risk of hitting the spinal cord with the needle. Penetration of the dura mater produces a subtle "pop" that is most easily detected with the pencil-point needles. Single-shot spinal anesthesia provides excellent pain relief for procedures of limited duration, such as cesarean delivery, the second stage of labor, rapidly progressing labor, and postpartum tubal ligation. A long-acting local anesthetic often is used, with or without an opioid agonist. The duration of anesthesia is approximately 30-250 minutes depending on the drugs used. However, because of its inability to extend the duration of action, single-shot spinal analgesia is of limited use for the management of labor. Combined spinal-epidural anesthesia (CSEA) is a useful technique by which a spinal block and an epidural catheter are placed simultaneously. This technique is growing in popularity because it combines the rapid onset, dense block of spinal anesthesia with the flexibility afforded by an epidural catheter. There are special epidural needles with a separate lumen to accommodate a spinal needle available for CSEA. The spinal component of CSEA may be an intrathecal narcotic plus a small amount of a local anesthetic. Failure of the spinal component occurs at a rate of 4% with CSEA, but the block can be supplemented with epidural catheter (3). Although CSEA shows great promise, additional, prospective studies are necessary to identify the relative risks and limitations of the technique. The absolute contraindication to spinal or epidural anesthesia is patient refusal. However, several pre-existing conditions increase the relative risk of these techniques, and the anesthesiologist must carefully weigh the expected benefits before proceeding. Some conditions that increase the risks are: Several retrospective studies have shown an increased risk of cesarean delivery in nulliparous women in whom epidural analgesia was administered before cervical dilatation of 4 cm or 5 cm. At this time it appears to be possible that very early placement of epidural analgesia may increase the risk of cesarean delivery and that the risk decreases with delayed epidural placement. After weighing this conflicting data, the ACOG Task Force on Cesarean Delivery Rates recommended that, when feasible, obstetric practitioners should delay the administration of epidural analgesia in nulliparous women until cervical dilatation reaches 4-5 cm and that other forms of analgesia be used that time. However, 4 cm of dilatation is an arbitrary cutoff because decreased risk with increased cervical dilatation is a continuum. Therefore, the decision of when to place epidural analgesia should be made individually with each patient, with other factors, such as parity, taken into consideration. Women in labor should not be required to reach 4-5 cm of cervical dilatation before receiving epidural analgesia (7). Regional anesthesia is preferred for women with preeclampsia and eclampsia; both for labor and delivery. General anesthesia carries more risk to pregnant women than does regional anesthesia. Regional analgesia in women with preeclampsia is associated with an overall 15-25% reduction in systemic mean arterial pressure. Although the peripheral vasodilation seen with regional analgesia may be helpful in decreasing severe hypertension, hypotension that requires cautious treatment with ephedrine may occur. In addition, prehydration with crystalloid combined with intraoperative fluid boluses for hypotension results in an average additional fluid challenge of 600-800 mL in women with preeclampsia receiving regional analgesia (8). There is sufficient evidence to address the safest level of maternal oral intake during labor. The ASA Task Force on Obstetric Anesthesia recommends allowing a modest intake of clear liquids in patients experiencing normal labor. However, fasting period of 6-8 hours for solids is preferable before elective cesarean delivery. For both elective and indicated cesarean delivery, agents to decrease gastric acidity should be used. Sodium citrate with citric acid has been shown to neutralize the gastric contents of 88.5% of women undergoing cesarean delivery and should be administered when the decision is made to perform cesarean delivery. Epidural and spinal anesthesia each have advantages and disadvantages that may make one or the other technique better suited to a particular patient or procedure. Controlled studies comparing both techniques for surgical anesthesia have consistently found that spinal anesthesia takes less time to perform, produces more rapid onset of better-quality sensory-motor block, and is associated with less pain during surgery. Despite these important advantages of spinal anesthesia, epidural anesthesia offers advantages, too. Chief among them are the lower risk of post-dural puncture headache (PDPH), less hypotension if epinephrine is not added to the local anesthetic, the ability to prolong or extend the block using an indwelling catheter, and the option of using an epidural catheter to provide post-operative analgesia. Regional analgesia is preferred in women with preeclampsia unless a contraindication to regional analgesia is present. Breast feeding does not appear to be affected by the choice of anesthesia; therefore, the choice should be based on other considerations. Identifying women with risk factors for failed intubation or other complications of anesthesia and referring them for antepartum anesthesia consultation may reduce this risk. To avoid respiratory depression, close monitoring for the cumulative narcotics dosage given to a patient antepartum, intrapartum, and postpartum is essential. The decision of when to place epidural analgesia should be made individually. |